Catheters and the Risk of Infection
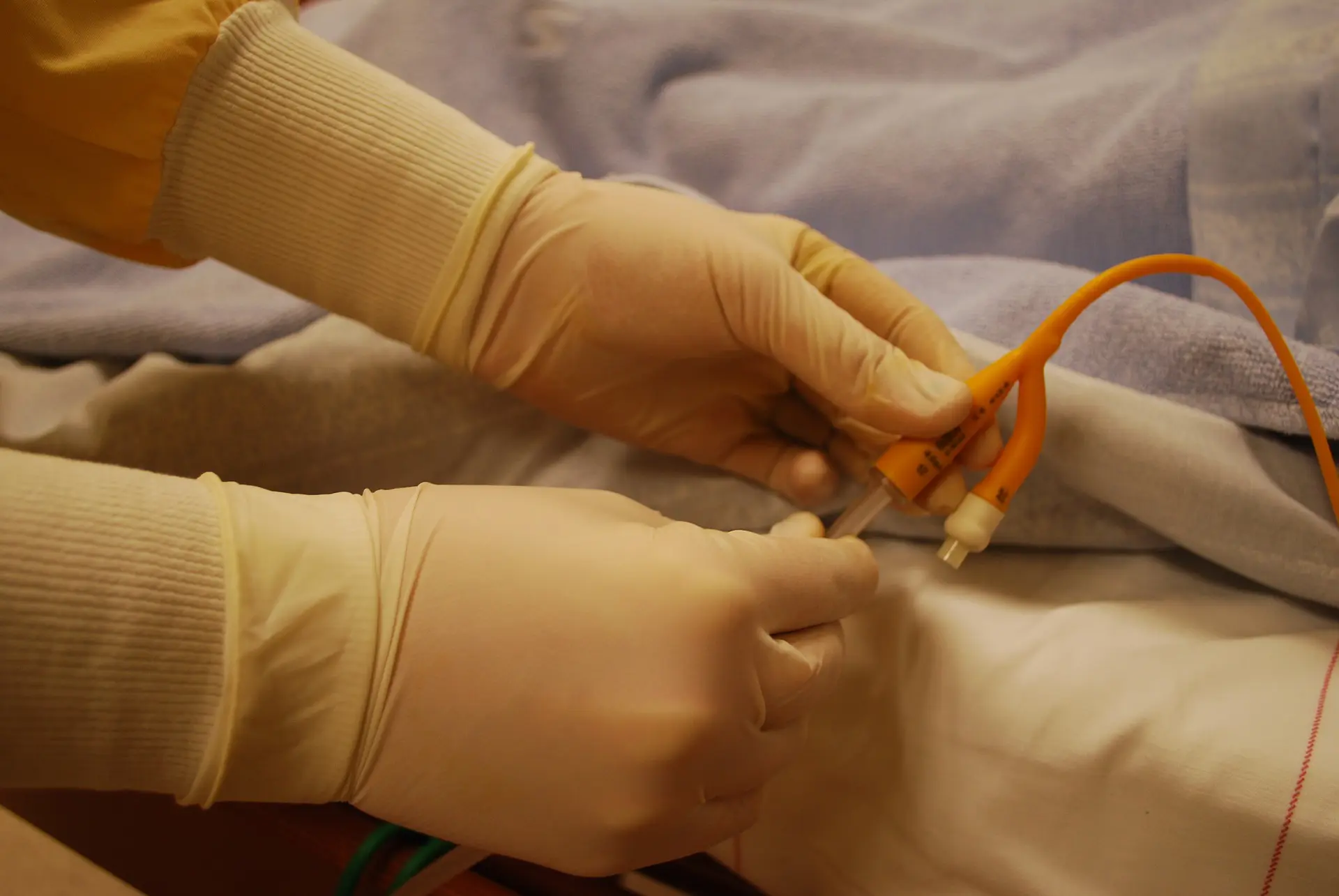
A July 2019 study published by the University of Michigan found that up to 25% of healthcare-associated infections (HAIs) are linked to indwelling devices like catheters. Worse yet, the study concluded that doctors and nurses’ failures to communicate were usually the cause of these infections.
To quote the article on ScienceDaily, “Even routine patient care such as catheter use can cause serious problems for patients if communication breaks down among health care workers.” Milisa Manojlovich, head of the School of Nursing at U-Mich, commented, “People get catheters all the time, but meanwhile they cause lots of harm so we need to talk about them. This study found a whole host of factors that affected the ability to discuss this issue.”
Leventhal Puga Braley P.C. has firsthand experience with the dangers patients face when healthcare providers are not engaged, mindful, and given strict procedures to follow. Let’s talk catheters.
How Catheters Can Harm Patients
All of those surveyed for this U-Mich study reported that poor communication was responsible for the delayed removal of “unnecessary” catheters. A few of the reasons they gave included:
- Catheters are often hidden beneath blankets, and a doctor on his rounds may not notice it or check the patient thoroughly – if a nurse isn’t present or doesn’t speak up, that patient may be stuck with a catheter longer than needed.
- Doctors and nurses don’t always get along, and this can lead to nurses having a reluctance to speak up, and for doctors to fail to ask questions. This kind of passive-aggressive avoidance can seriously harm patients.
- Nurses aren’t always scheduled to be present when doctors, surgeons, and administrators make patient care plans. However, nurses often have the most up-to-date and on-the-ground knowledge about the patient’s actual condition.
- Medical records are not always kept up-to-date, and there’s often a lag or disconnect between the electronic record and the paper record – many hospitals still have both, and do not have thorough guidelines for who, how, and when they should be updated.
- Patients are often given catheters as a matter of course to remove the obstacle of the patient having to get up (and perhaps need assistance) using the bathroom, and some patients and their families request them. But patients and their families should be warned that catheters come with elevated risks of infection, pain, physical trauma, and bleeding – sometimes even more complications.
Catheters are medical devices, similar in a sense to hip replacements and pacemakers. They are non-organic, supposedly sterile objects that are inserted inside the body, and any foreign object in the body carries an infection risk. In addition, catheters create a “superhighway” for bacteria to enter the bladder, the bloodstream, or another part of the body if hospital workers do not keep them (and the area around them) clean.
Urinary Tract Infections Are the Most Common
The study estimated that 60% to 90% of intensive care patients, and 10% to 30% of those outside the ICU, have urinary catheters in place. And catheter-associated urinary tract infections (CAUTIs) may be the most common infection people contract in the hospital, according to the American Association of Critical-Care Nurses. If the catheter was not sanitized before insertion, is not regularly emptied and cleaned, the fill bag overflows and urine goes back into the bladder, or the catheter is left in too long, you have a very good chance of developing a CAUTI.
Is this medical malpractice? If a patient develops an infection around a urinary catheter due to a nurse’s poor sanitation practices, requiring additional medication and worsening an already-delicate health condition, that’s a yes. If the patient contracts a CAUTI and it goes untreated due to the hospital administrators choosing to understaff the ward, becoming a system-wide case of sepsis, requiring emergency measures to save the patient’s life, that’s a definite yes.
Negligence – a breach in the standard of care a medical professional is required to provide to a patient – is required for a medical malpractice lawsuit. However, that doesn’t mean every claim is a strong one. These lawsuits are really meant for people who are seriously harmed, whose health is made provably worse, by something even other doctors will admit was a “mistake” in standard operating procedure or judgment. That’s what our law firm proves in court all the time.
We don’t call it a mistake. We call it a failure to do your job when people’s lives are at stake.
Why HAIs Shouldn’t Be Happening
Medical devices, especially tubing and insertions and implants, have serious risks already, as we discussed in our last blog on medical device miscommunication. Hospitals have a duty to make sure patients are not harmed by the treatment itself. Especially when such infections could easily be prevented!
In early 2018, Leventhal Puga Braley P.C., started taking cases involving Porter Adventist Hospital in Denver. It was discovered that Porter was failing to properly sterilize its surgical equipment, resulting in instruments having retained biological material and bacteria, and thousands of patients were exposed to bloodborne pathogens and severe infections. We represented a doctor from that very hospital who had her surgery there and contracted a serious infection.
We want to drive home how much responsibility hospitals have in preventing this kind of negligence – but we don’t forget the doctor’s role in checking up on his/her patient, and the nurse’s role in communicating changes to the attending physician. Many professionals have a part to play in modern healthcare, and when one of them fails, the patient can be left with devastating internal organ damage, or worse.
If you contracted a serious infection while in hospital care, do not hesitate to contact us at (877) 433-3906. Our trial lawyers handle medical malpractice claims across the United States, and we can look into your records and see if you were given the standard of care you deserved. Your initial consultation is free, and if we take your case, we front the costs and do not take payment until we win a jury verdict or settle out of court.
Read about the U-Mich study here.